There is no doubt that changing lifestyle and dietary habits have led to rising obesity levels in Asia Pacific, with two of every five adults in the region either overweight or obese1. In recent years, Non-alcoholic fatty liver disease (NAFLD), linked with fatty foods and obesity, has become more prominent in this part of the world2, and with it, so has liver disease.
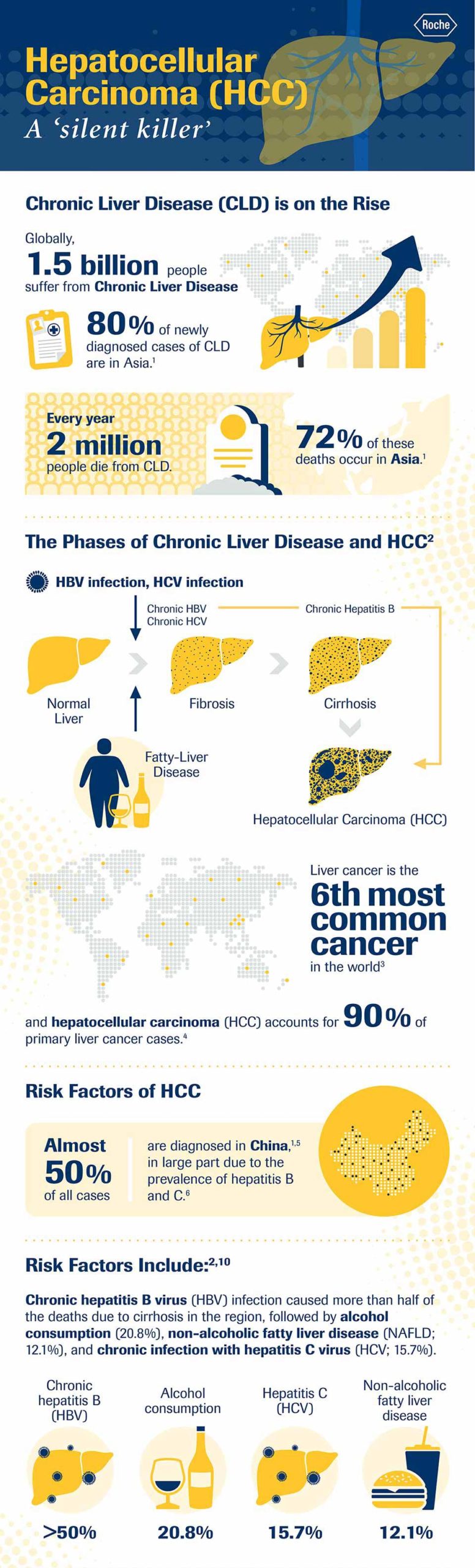
Symptoms of chronic liver disease can often be vague and misleading, becoming obvious only after there has been extensive damage to the liver. By this time, it can lead to severe fibrosis or cirrhosis or worse still, progress to liver cancer, also called hepatocellular carcinoma (HCC). While there are several risk factors for HCC, hepatitis3 – known to cause inflammation of the liver – is one of the most common.
Viral hepatitis remains a major public health concern in the region and is largely unchecked. According to estimates, Asia Pacific has two-thirds of the global viral hepatitis burden4. Viral hepatitis B and C have a high prevalence in most countries in Asia3 – with Japan being an exception where hepatitis C is a major cause5. The high hepatitis prevalence directly contributes to the higher incidence of HCC in the region3.
Related read: Breaking Boundaries in Indonesia’s Cancer Care
President of The Asian Pacific Association for the Study of the Liver (APASL) and a leading expert in the field of hepatology, Dr Tawesak Tanwandee, puts this down to a gap in understanding. “There is tremendous need to elevate awareness and knowledge of liver diseases among the general public, the medical community and policy makers. It is largely seen as a specific disease-related topic instead of the growing public health issue that it is.”
As part of its efforts, APASL focuses on medical education, public awareness campaigns and coordinating scientific studies across the region. Chief among these is establishing consensus through the development of guidelines to ensure a common standard of care in the region.
“Where a liver disease patient lives should not determine the standard of care he or she receives. Our aim is to create a minimum acceptable standard that prolongs survival and ensures quality of life of these patients.”
Value Based Care Means Better Outcomes and Cost Savings

The historical model of healthcare spending has primarily considered cost factors, but Dr Tanwandee cites the example of Thailand, where he is based, to explain how a shift towards value-based healthcare can illustrate the benefits in both cost savings as well as cost effectiveness terms. “The government has implemented several initiatives over the years to promote evidence-based policy decisions. One such example is through the introduction of economic appraisals within health information and technology assessment program (HITAP). For any treatment or test to be included in our national guidelines, they have to go through a cost effectiveness study”.
“The goal is to assess the cost per quality-adjusted life years (QALY) and determine whether such diagnostic interventions or therapy bring value to patients and the healthcare system,” he adds. “We have done this for chronic viral hepatitis too.”
Explore more inspirational medical stories.
The Thai Government has set itself a target of eliminating hepatitis C by 2030 in accordance with the WHO target6 by launching efforts to minimise transmission, offering free hepatitis B and C screening to citizens and introducing targeted therapies in its Universal Health Coverage program.
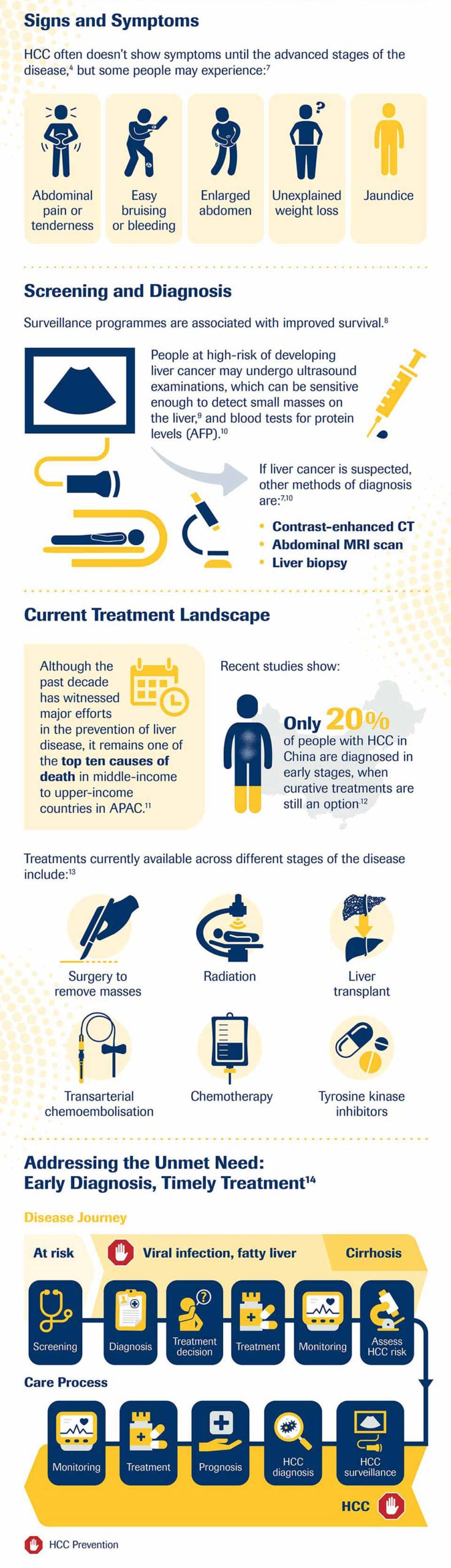
The screening and diagnosis of hepatitis infections are key components of an effective response to reducing the liver cancer burden. Early identification of persons with chronic HBV (hepatitis B virus) or HCV (hepatitis C virus) infection enables them to receive necessary care and treatment, thus delaying the progression to HCC.
Revolutionising Care by Moving Towards Early Interventions
Globally, chronic hepatitis B accounts for approximately 50 percent of all cases of HCC7. “Once the disease has significantly progressed, there is a huge economic impact on patients and their families due to the long hospitalisation and cost of treatment. This becomes a barrier for most patients,” adds Dr Tawesak.
Inadequate infrastructure and insufficient healthcare personnel trained in hepatology are other factors that become detrimental to patient care. Almost 85 percent of HCC cases are estimated to occur in low-resource or middle-resource countries8, particularly in Eastern Asia and sub-Saharan Africa, where medical resources are often limited.
Many cases of liver cancer are often diagnosed at an advanced stage. Less than 50 percent of people with advanced HCC will survive more than a year after diagnosis9. If diagnosed early, it may be possible to cure the cancer completely10.
Prevention Should be the Goal
With HCC surveillance mechanisms in place, health authorities can periodically test at-risk populations, detect HCC occurrence at an early stage to allow for curative intervention. Together with a comprehensive approach that includes vaccination, improved risk stratification and the use of newer, more advanced hepatitis therapies, the burden in Asia Pacific can be considerably reduced – giving patients a better future.
Stay updated on healthcare and diagnostics news with Diagram magazine.
References:
1Asian Development Bank Institute (ADBI): Fighting Obesity in Asia and the Pacific Policy Brief
2Wong SW, Ting YW, Chan WK. Epidemiology of non-alcoholic fatty liver disease-related hepatocellular carcinoma and its implications. JGH Open. 2018;2(5):235–241.
3Tanaka, M., Katayama, F., et al. Hepatitis B and C Virus Infection and Hepatocellular Carcinoma in China: A Review of Epidemiology and Control Measures. Journal of Epidemiology. 2011;21(6):401-416.
4Moon Am, et al. Clin Gastroenterol Hepatol. 2019 Aug
5JP reference
6Combating hepatitis B and C to reach elimination by 2030: WHO Advocacy brief
7HB El-Serag. Epidemiology of Viral Hepatitis and Hepatocellular Carcinoma. 2012
8Yang et al. Nature Reviews Gastroenterology & Hepatology volume 16, pages589–604(2019)
9Giannini EG et al. Prognosis of Untreated Hepatocellular Carcinoma. Hepatology. 2015;61(1):184-190.
10Llovet et al. Hepatocellular carcinoma. Nat Rev Dis Primers. 2016;2:16018.
References (Micrographics)
1Moon Am, et al. Clin Gastroenterol Hepatol. 2019 Aug
2Omata et al. APASL guideline Hepatol Int (2017) 11:317–370
3WHO: Globocan 2018 – Liver cancer factsheet. [Internet; cited 2019 July 24] Available from: http://gco.iarc.fr/today/data/factsheets/cancers/11-Liver-fact-sheet.pdf
4Llovet J, et al. Hepatocellular carcinoma. Nat Rev Dis Primers. 2016;2:16018.
5WHO: Globocan 2018 – China cancer factsheet. [Internet; cited 2019 July 24] Available from: http://gco.iarc.fr/today/data/factsheets/populations/160-china-fact-sheets.pdf
6Tanaka M, et al. Hepatitis B and C Virus Infection and Hepatocellular Carcinoma in China: A Review of Epidemiology and Control Measures. J Epidemiol. 2011;21(6):401-416.
7Medline. [Internet; cited 2019 July 24]. Available from: https://medlineplus.gov/ency/article/000280.htm
8Giannini G, et al. Prognosis of untreated hepatocellular carcinoma. Hepatology. 2015;61(1):184-190.
9Medscape. [Internet; cited 2019 July 24]. Available from: https://emedicine.medscape.com/article/369226-overview
10Omata et al. APASL guideline Hepatol Int (2017_ 11:317-370)
11World Health Organization. The top 10 causes of death in 2015. WHO http://www.who.int/mediacentre/factsheets/fs310/en/index1.html (2016).
12Wu Q, Qin S. Features and treatment options of Chinese hepatocellular Carcinoma. Chin Clin Oncol. 2013;2(4):38.
13Marrero K, Kulik L, et al. Diagnosis, staging, and management of hepatocellular carcinoma: 2018 practice guidance by the American Association for the Study of Liver Diseases. Hepatology. 2018;68(2):723-750.
14Zhao et al. Liver International 2018; 38: 503-514
Date of preparation: September 2020














