
COVID-19 has brought diagnostics to the world stage, ushering labs into the spotlight.
Despite our experiences from previous pandemics, Dr Ravindran Thayan, Head of Virology Unit, Infectious Diseases Research Centre, Institute for Medical Research (IMR), Kuala Lumpur, Malaysia says that many laboratories across the region weren’t equipped for the surge in testing due to COVID-19. True preparation, he adds, requires robust and consistent improvement across labs on a national level.
“It’s important to equip both rural and centralised labs across the country so we can decentralise testing with appropriate risk mitigation steps. The ability to ramp up testing quickly allows governments to develop effective containment strategies to deal with pandemics effectively and efficiently,” explains Dr Thayan.
Healthcare’s Intelligence Unit
The success or failure in pandemic management can hinge on one space: the lab.
COVID-19, SARS and the H1N1 flu (also known as “swine flu”) have shown that diagnostics do far more than simply confirm results. By aggregating the data derived from labs, countries like Singapore1 and Taiwan2 have been able to quickly identify clusters, which inform where to focus efforts to contain outbreaks.
As evidenced, an effective pandemic response strategy is supported by robust testing capabilities. Yet in labs, these capabilities are impacted by myriad factors spanning regulation, access to technology and reagents, and human technicians — factors that differ hugely between developed and emerging countries.

Dr Abdul Bari Khan (centre) is co-founder and CEO of Indus Hospital, in Pakistan.
Addressing Inherent Challenges
“The biggest gaps are inequities in the availability and accessibility of healthcare, including laboratory services,” says Dr Abdul Bari Khan, co-founder and CEO of Indus Hospital in Pakistan. “At a country-wide level, these problems can be addressed by improving the public health system and encouraging public-private partnership models which aim to deliver free or subsidised healthcare.”
At a regional level, Dr Thayan calls for ”pandemic-proof” supply chains that ensure consistent flow of essential regents, kits, and protective equipment for labs to continue operations. “With the lockdowns and countries closing their borders because of COVID-19, that was a huge challenge for laboratories. Countries, and therefore labs, are so interdependent on one another. We had to source for reagents from different suppliers in such a short amount of time, just to make sure we had a steady supply to manage the testing load. Thankfully we had enough resources to scale up testing when required.”
On a global level, strengthening the capabilities of labs comes down to collaboration and capacity, Dr Khan notes. “With countries supporting each other, we can reduce the global reaction time to implement an effective strategy for pandemic control.” As such, he stresses, “Capacity development in countries less prepared to deal with the pandemic needs to be prioritised.”
Related read: Understanding COVID-19 Testing

“Smarter” Testing Strategies to Overcome Limited Resources
Some developing economies, however, have not been able to expand their testing capacities as quickly. Many struggle to access the diagnostic tests needed due to limitations in resources, support and regulations.3 For instance, the polymerase chain reaction tests which are considered the most reliable form of diagnostic for COVID-19 are costly to administer4 and require specialised equipment to process.5 Emerging labs have had to pivot to “smarter” testing strategies because of these limitations.
One viable alternative for prompt diagnosis is rapid test kits, offering fast portable point-of-care testing.6 This not only saves time, but allows diagnostics to be taken to villages and smaller towns, where access to testing is far more limited.
Similarly in Malaysia, Dr Thayan says his organisation is also looking into the possibility of “plug and play” mobile labs for areas with limited access to testing, or at entry points such as airports. “While molecular testing will still be the ‘gold standard’ of testing, we need to think about ways to make testing more accessible and mobile. You want the test to be immediate so that once you know a person is positive, you can then manage and contain them quickly,” he explains.
The Power of Automation
With the flood of samples that need processing and the prevalence of staff fatigue,7 human-induced errors in labs are inevitable, especially during a pandemic. This can lead to contagious people being cleared as COVID-free.
As such, experts are calling for more rigorous lab processes, from adoption of barcode testing to interfacing with electronic patient medical records. However, even for low-resource labs, simple changes to training, such as incentivising staff to find and report any labelling errors they spot,8 can make a difference.
In high-resource labs, automation allows for greater quantities of tests to be processed while reducing human error and lab infection.9
“With increasing demand, automation becoming almost indispensable, lab workers need to be trained in the handling of technology and managerial skills, as well as administrative techniques,” says Dr Khan. These, he says, will be more in demand as automation dispenses with technical human skills.
According to Dr Thayan, automating a lab is a good opportunity to improve its workflow and efficacy. He adds, “It also frees up our technicians who can then be developed and trained to manage a lab, probably in a part of our country that requires more resources. As part of future-planning, this is an effective strategy to build up the lab infrastructure across a country, and bring testing capabilities to areas that severely need it.”
Read more about the latest in innovative diagnostic laboratory solutions.
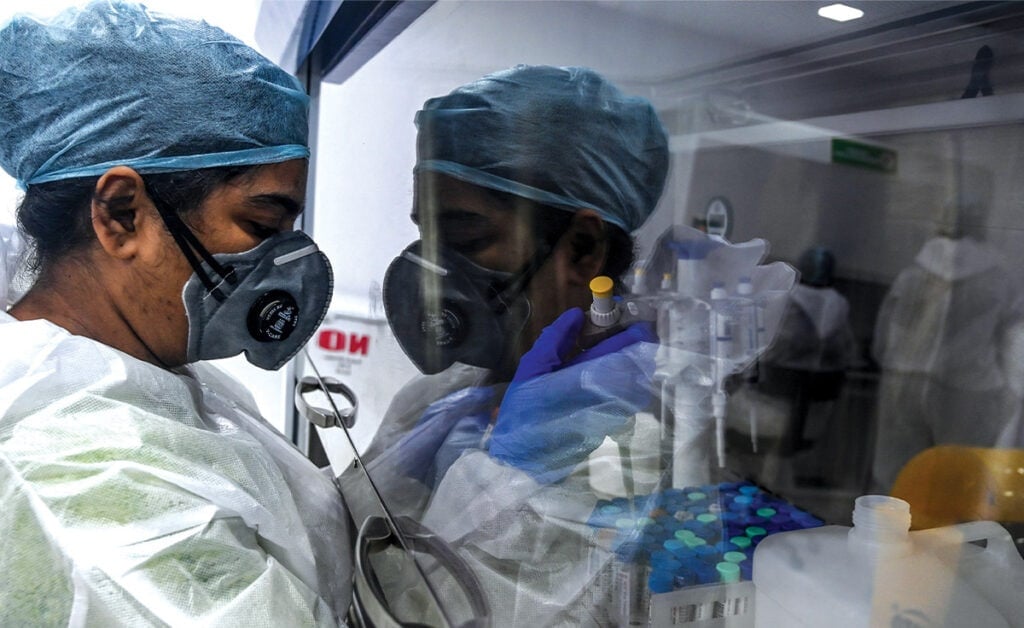
There is an opportunity for testing labs to revolutionise their role and become the keystone of national health strategies, particularly in times of a pandemic.
A Pivotal Partner: Advancing the Role of Laboratories
The shift to move away from “result generators” to “data aggregators” has been in the making for a while now but the peri- and post-pandemic world has perhaps accelerated the need for labs to be front runners in this new age of healthcare.
At each stage of pandemic management, the lab holds intelligence gathered from patient data on a national scale. This can provide policymakers and clinicians with key insights they need to make the right decisions. “From early detection, screening populations, monitoring disease progression, and even assessing the efficacy of a vaccine — the lab is always there. It’s up to us to advocate for continuous development and improvement of laboratories. What we do today will determine how prepared we are for tomorrow,” says Dr Thayan.
Keep up with the latest developments in healthcare and diagnostics news with Roche Diagram.
References:
1Yong S, Anderson D, Wei W, et al. (2020). Connecting clusters of COVID-19: an epidemiological and serological investigation. The Lancet Infectious Diseases, 20(7), 809-815. https://doi.org/10.1016/S1473-3099(20)30273-5
2Cheng H Y, Li S Y, and Yang, C H. (2020). Initial rapid and proactive response for the COVID-19 outbreak – Taiwan’s experience. Journal of the Formosan Medical Association Taiwan yi zhi, 119(4), 771–773. https://doi.org/10.1016/j.jfma.2020.03.007
3McNerney R. (2015). Diagnostics for Developing Countries. Diagnostics (Basel, Switzerland), 5(2), 200–209. https://doi.org/10.3390/diagnostics5020200
4Knight G M, Dyakova E, Mookerjee S. et al. (2018). Fast and expensive (PCR) or cheap and slow (culture)? A mathematical modelling study to explore screening for carbapenem resistance in UK hospitals. BMC Medicine, 16(141). https://doi.org/10.1186/s12916-018-1117-4
5Behnam M, Dey, A, Gambell T, and Talwar V. (2020). COVID-19: Overcoming supply shortages for diagnostic testing. McKinsey & Company. Retrieved from https://www.mckinsey.com/industries/pharmaceuticals-and-medical-products/our-insights/covid-19-overcoming-supply-shortages-for-diagnostic-testing
6Kobia F, and Gitaka J. (2020). COVID-19: Are Africa’s diagnostic challenges blunting response effectiveness? AAS Open Research, 3, 4. https://doi.org/10.12688/aasopenres.13061.1
7Tan SS, Yan B, Saw S, et al. (2020). Practical laboratory considerations amidst the COVID-19 outbreak: early experience from Singapore. Journal of Clinical Pathology. https://doi.org/10.1136/jclinpath-2020-206563
8Scott K. (2020). Advancing Standards for Specimen Labeling and Tracking. American Association for Clinical Chemistry. Retrieved from https://www.aacc.org/cln/articles/2020/june/advancing-standards-for-specimen-labeling-and-tracking
9Ford B A, and McElvania E. (2020). Machine learning takes laboratory automation to the next level. Journal of Clinical Microbiology. 58:e00012-20. https://doi.org/10.1128/JCM.00012-20
10 Centers for Disease Control and Prevention, COVID-19 Forecasts: Cases, 2020. https://www.cdc.gov/coronavirus/2019-ncov/cases-updates/forecasts-cases.html














