
Professor Christian Müller of the University Hospital of Basel, Switzerland, is actively involved in cardiovascular biomarker research and is the Principal Investigator of the TRAPID-AMI study. He is a professor at the Swiss National Science foundation, won several awards for his achievements in cardiology research and is an editor of the European Heart Journal as well as the Journal of the American College of Cardiology.
Acute myocardial infarction (AMI) is a condition where minutes count, with delays to treatment as short as half an hour having a measurable effect on a patient’s chance of long-term survival. The TRAPID-AMI (High sensitivity cardiac troponin T assay for RAPID rule-out of Acute Myocardial Infarction) study1 was published in the Annals of Emergency Medicine earlier this year, confirming a novel approach for a more rapid diagnosis of heart attack in patients with acute chest pain. The strategy is based on the cardiac troponin T high-sensitivity test and reduces the observation time needed to rule-in or rule-out a heart attack from 3-6 hours to just 1 hour. The European Society of Cardiology adopted this accelerated diagnostic concept at their annual meeting held in London (UK) in August 2015. Their new clinical practice guidelines (2015 ESC NSTEMI) now support the 1-hour diagnostic algorithm with high-sensitive troponin testing validated in the TRAPID-AMI study2 and other studies such as APACE.3
Prof Christian Müller of the University Hospital of Basel, Switzerland, Principal Investigator of TRAPID-AMI study, gave us insights into how patients and physicians in the emergency department (ED) will benefit.
This is of critical help in the allocation of resources in emergency departments.
How do the results of the TRAPID-AMI study have the potential to change clinical practice?
With conventional assays, guidelines recommend measurements at presentation and after six hours. So everybody would have to wait for six hours in the ED for the second measurement to make sure the patient was not having an AMI. With the use of high-sensitivity assays, the guidelines of the European Society of Cardiology recommend that the second measurement can be done after three hours.
But that still means we have to wait for three hours to do the second measurement, and only then can we be sure whether or not the patient has had an AMI. The beauty of the one-hour algorithm is that we can accelerate our diagnostic procedure and in 75% of patients obtain the same information after one hour. This tells us whether or not the patient can be ruled out for AMI or has a very high likelihood of having AMI.
Who will benefit from the results of this study? Patients, emergency departments, cardiologists?
Ultimately, I strongly hope everybody. It’s a great benefit for the patient, we think using the algorithm in clinical practice will allow improvement in patient care. It will be of huge operational benefit in the ED. If a patient with a benign, non-cardiac disease occupies a room in the ED for six hours then that room cannot be used for other patients with acute life-threatening disorders. And of course we cardiologists will have a substantial benefit because the algorithm really makes best use of the diagnostic information provided by the cardiac troponin assay. However, while the algorithm does a fantastic job, it must always be applied in conjunction with the proper clinical assessment including a 12-lead electrocardiogram (ECG).
The beauty of the one-hour algorithm is that we can accelerate our diagnostic procedure.
Could the introduction of this one-hour algorithm to clinical practice help reduce overcrowding in the emergency department?
Overcrowding is a major issue in many EDs all over the world. I really think that the application of this one-hour algorithm will help to reduce overcrowding because it reduces the time to diagnosis, particularly for those patients who are at extremely low risk and do not have an acute life-threatening disorder but a benign disorder.
At the hospital level, could we anticipate any financial impact associated with the application of the TRAPID-AMI one-hour algorithm?
It is extremely likely that the clinical application of the one-hour algorithm will be associated with a substantial reduction in treatment cost because the most important driver of treatment cost in the ED is the duration of stay.
References:
¹Mueller, C., et al. 2015. Ann Emerg Med 68(1):76-87.e4.
²Roffi, M., et al. 2016. Eur Heart J 37(3):267-315.
³Reichlin, T., et al. 2015. CMAJ 187(8):E243-E252.
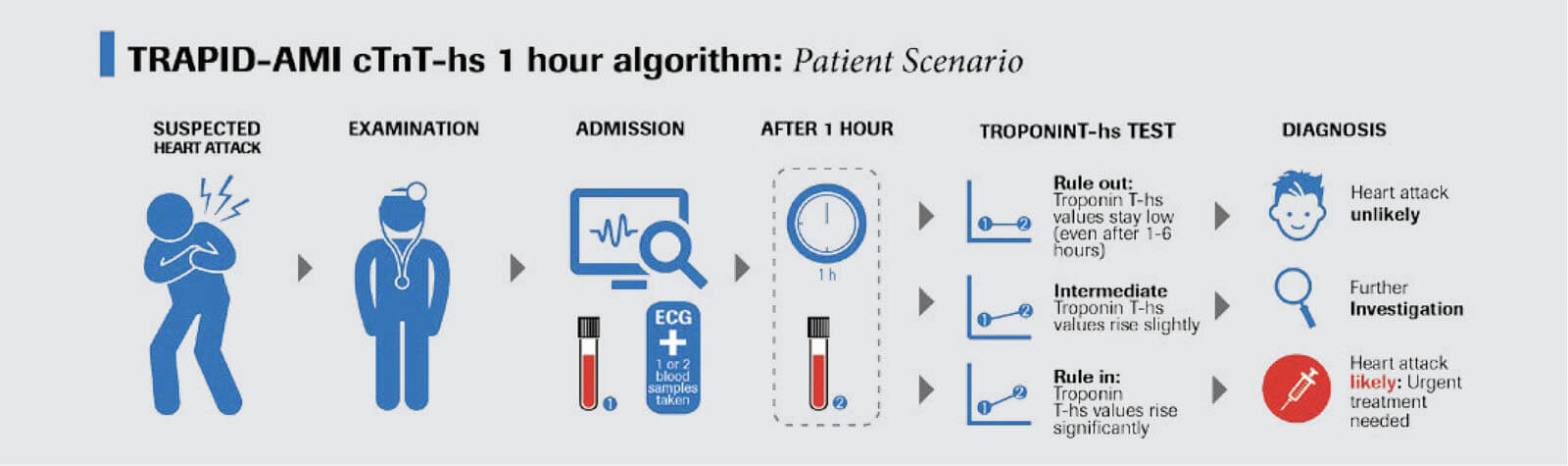
Infographic Reference:
Mueller, C., et al. 2015. Ann Emerg Med 68(1): 76-87.e4.














