The world of healthcare policy lives within a complex, untenable system that can make effective policy design and implementation a herculean task. COVID-19 has shown that among a slew of health outcome indicators, health utilisation must become a key priority. Rather than letting healthcare policies drift into a bureaucratic vacuum, governments are now beginning to assess ways in which the use of services to prevent and treat health problems, and the finite resources available to provide them, can be better managed.

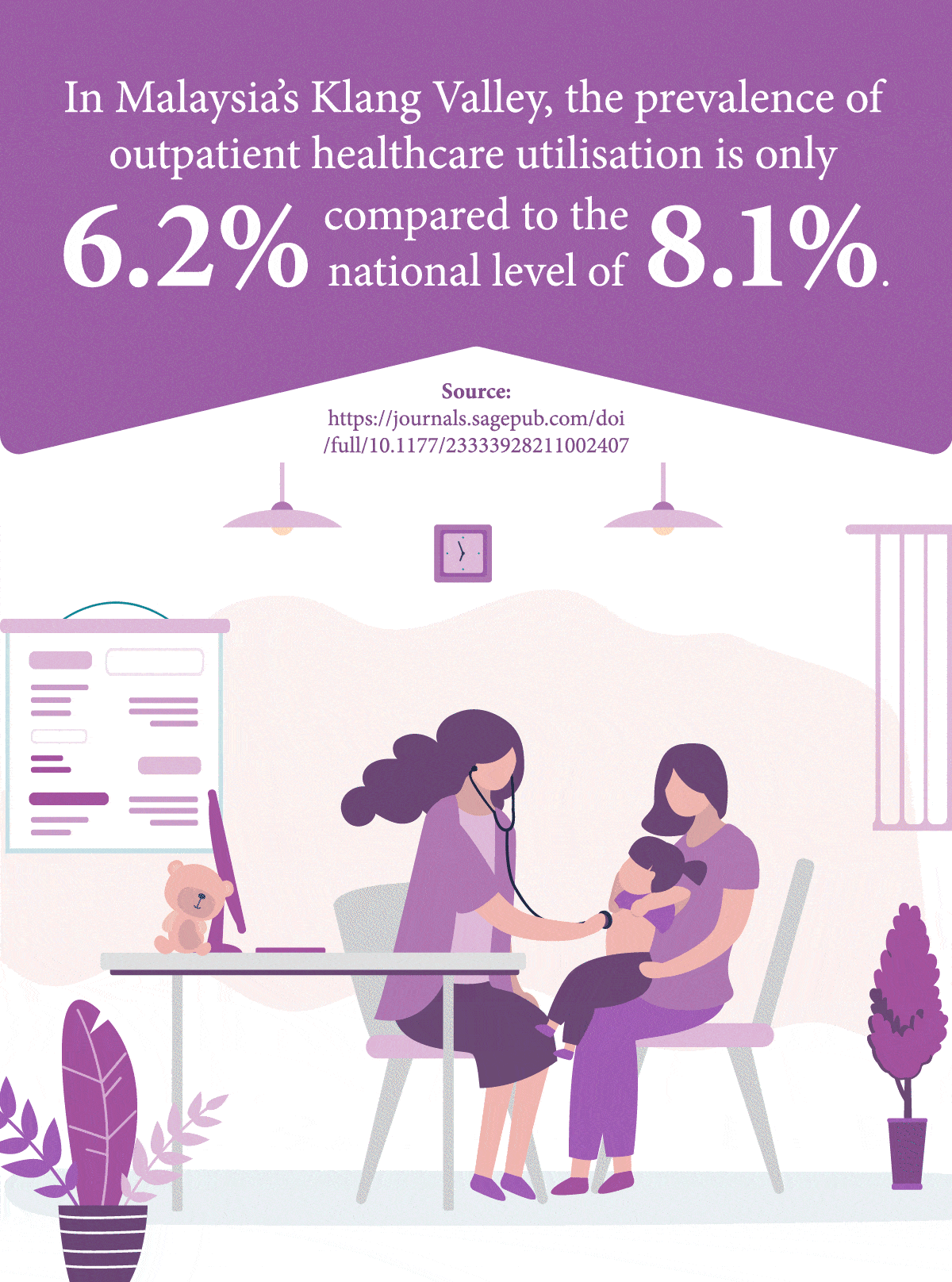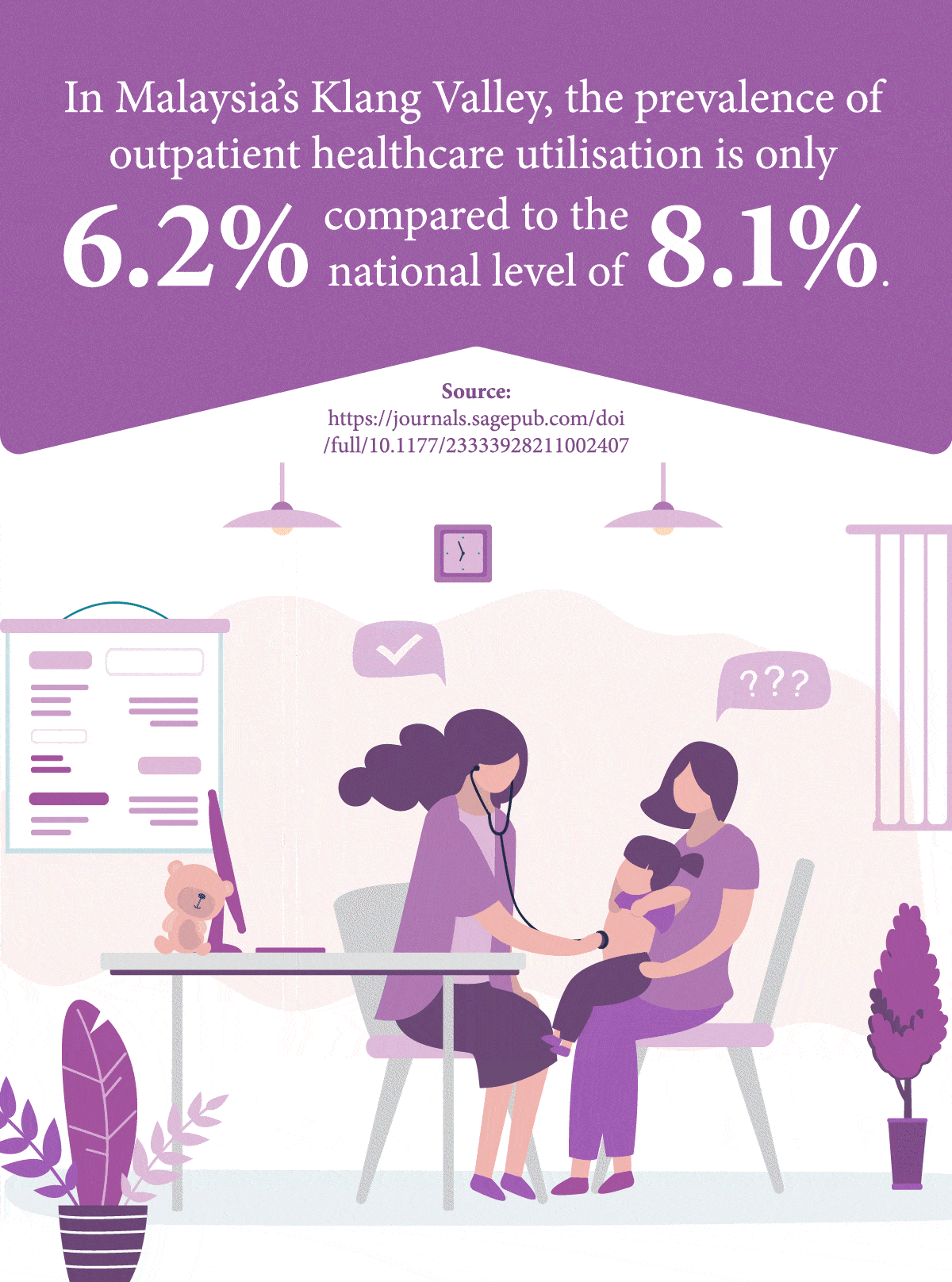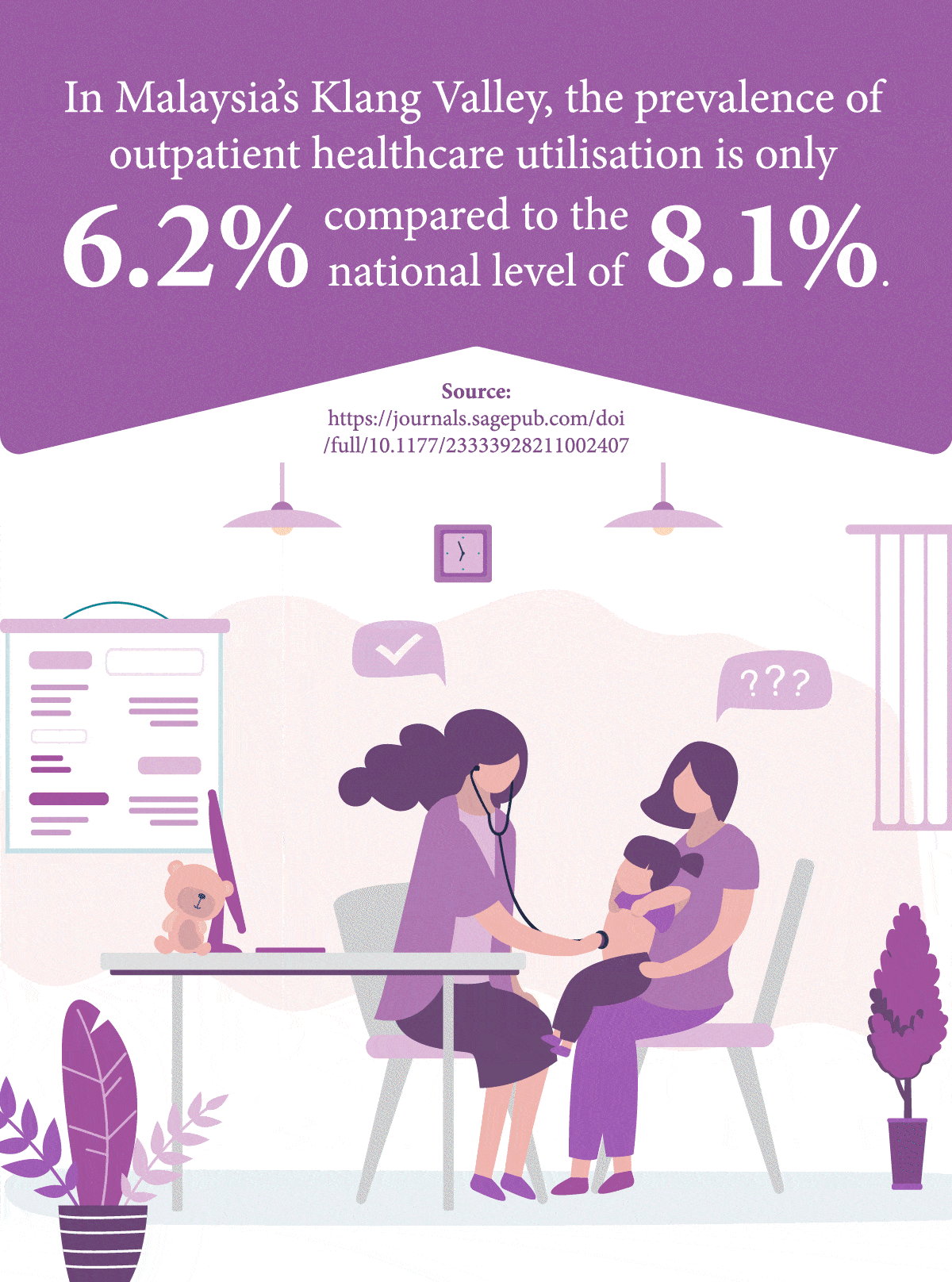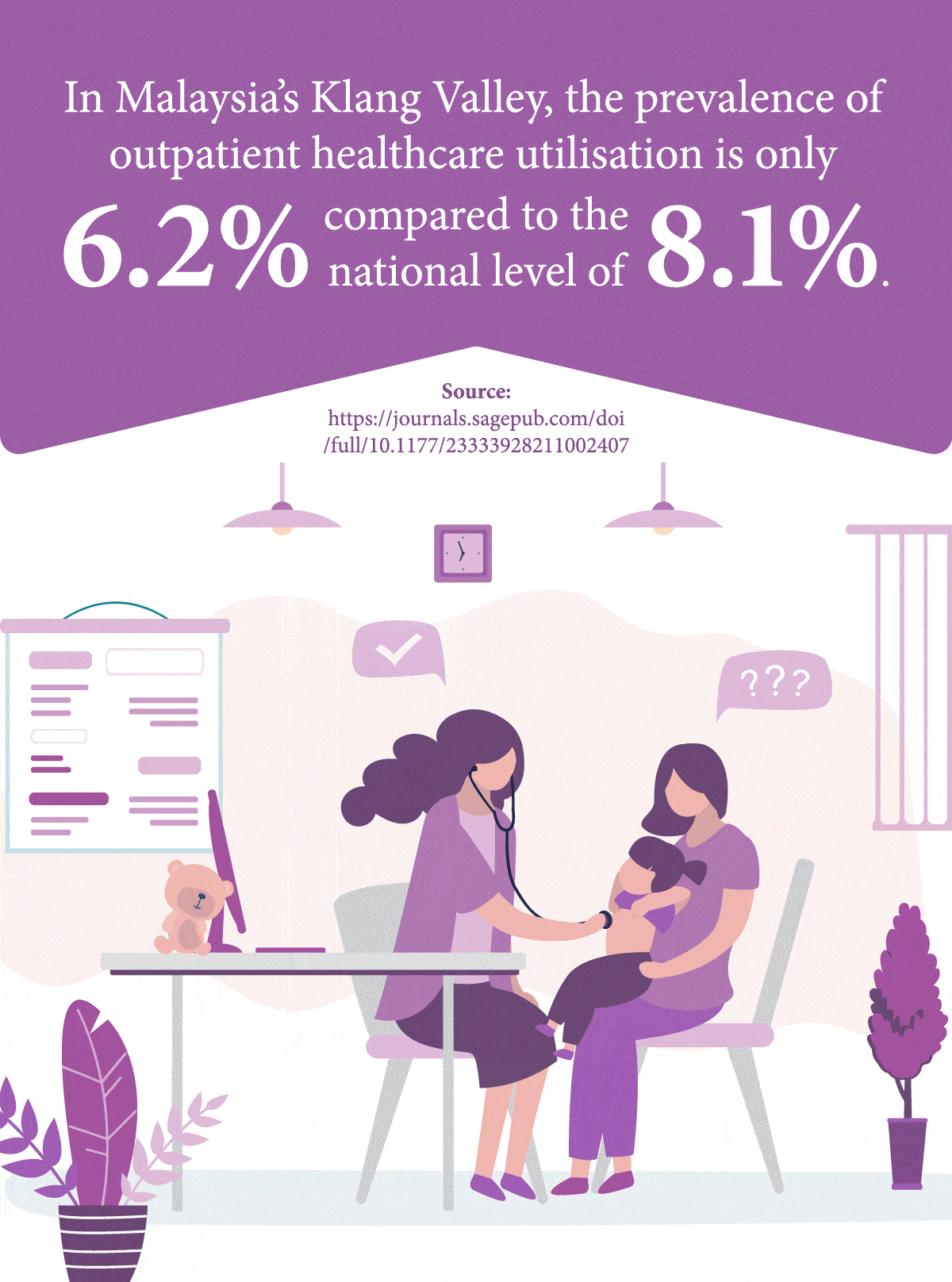
Compared to high-income countries, Malaysia’s level of healthcare utilisation services is relatively low1 – a problem especially magnified among people lower down the socioeconomic ladder who are more likely to suffer from inadequate access to care services, thus resulting in delayed diagnosis and treatment.
“This is where”, says Datuk Dr Zainal Ariffin Omar, President of the Malaysian Public Health Physicians Association, “health policymakers have a critical role to play in ensuring fair and equal access to all communities.”
Four areas of focus in particular stand out.
1. Building a More Inclusive Society
Malaysia’s public sector is currently facing greater constraints, exacerbated by the pandemic and rising healthcare costs. But in alignment with the United Nations’ goal of building a fairer,2 inclusive society,3 equal access to healthcare can ensure each Malaysian has a better chance at a better quality of life and good health, regardless of their socioeconomic status. It’s a move that can also save governments money in the long run as public health improves.
However, enhancing a single aspect of health utilisation is rarely enough. Improving a cancer patient’s access to hospital services, for instance, is only helpful if there are trained oncologists and nurses available with the essential tools. Likewise, improving access to a diagnostic test for a disease is effective — but only if it is complemented by educating staff and raising awareness among the population.
According to Datuk Dr Zainal Ariffin Omar, Malaysia will need a two-pronged approach in tackling NCDs. One is in early detection, where the aim is to provide quality and affordable screening tests for poorer citizens with NCD health issues such as diabetes and hypertension. “The next step is to look at areas outside these major towns, where it is much harder to monitor or follow up with patients in rural and less accessible locations,” he says.
2. Bringing Telehealth to the Masses
The country is looking at an alternative model — telemedicine4 — to provide the rural population with healthcare through the use of technology. It will enable them, for example, to receive check-ups without the need to travel outside their homes. At a low or fixed co-pay fee, patients can download the relevant app and connect with a doctor or specialist for a virtual consultation. Telemedicine not only benefits rural dwellers, but it also enhances urban healthcare by reducing referrals and crowding of medical facilities — vital benefits in a time of ever-changing COVID-19 strains.
But to incorporate telemedicine, Malaysia will first need to overcome a few barriers. Most crucially, the technology requires adequate bandwidth for videoconferences. Many rural areas do not have access to electricity, much less internet access for telemedicine. To even begin building a telemedicine foundation, infrastructure improvements are critically needed. As of 2019, 20 percent of the population still lacks access to the internet.5
“Our resources are stretched at the moment, but we are still looking into telehealth as it is an important component of our healthcare programme. It is an ongoing effort to support our medical centres in diagnostic screening,” says Datuk Dr Zainal.

3. Health System Preparedness Should be a National Priority
Since the onset of COVID-19, Malaysia’s response to the pandemic has been hampered by a rapidly mutating virus. Even initiatives outlined in the Strategic Framework of the Medical Programme (2021-2025) report, such as strengthening the stewardship of healthcare systems,6 will have to wait.
“We have various health plans and reform plans in place,” says Datuk Dr Zainal. “However, many of these have yet to be initiated due to COVID-19 and ongoing changes happening within the government. As much as we would like to work on these reforms, the focus now is more on pandemic management.” He stresses that while pandemic measures are vital, the country can’t ignore other burning healthcare issues.
Healthy financing to support the population’s health needs is also critical. Malaysia’s Ministry of Health has a total budget of almost RM32 billion7 for 2022.8 Its year-on-year increase, however, is only 4.3 percent, the lowest upturn in three years. “Even though we have an increase in the health budget in terms of volume, we need more resources in two key areas. One is to address NCDs, which is a problem in Malaysia, and the other is to focus on geriatric programmes,” Datuk Dr Zainal says. Based on current projections, Malaysia will be an aging nation by 2030,9 where the number of older citizens age 60 and above are expected to reach approximately 5.8 million — a hefty 15 percent of the total population.

4. Ensuring a Lasting Impact on Society
Recognising there is no single solution, Datuk Dr Zainal says health system stakeholders must work together to improve the lives of patients everywhere.
Circling back to the topic of screening and diagnostic testing, he says “extending and empowering diagnostic reach has the potential to reduce the immense strain on hospitals’ resources”, citing the example of point-of-care (POC)10 or near-patient testing as an area where innovative diagnostic solutions can positively impact patient health for those dwelling in the outskirts.
With analysis performed close to or near the patient, POC testing enables physicians and medical staff to accurately obtain real-time results within minutes, instead of hours or days.
As Datuk Dr Zainal explains, “We need to increase the modality of diagnostic tests. With the advancement of POC technology in recent years, we can now offer similar lab-quality and easy-to-use diagnostics in peripheral regions.”
Creating sound policy that helps invest in these measures will be a game-changer for the country, he concludes. “A well-planned healthcare policy, when effectively executed, has the capacity to transform the way we approach patient care and improve health outcomes for citizens who need access the most. There are visible challenges ahead, but we can’t let these obstacles derail our efforts.”
Diagram Dialogues
Subscribe to our podcast to hear expert insights from the world of diagnostics
References:
1Yunus, S., Puteh, S., Daud, A. (2021). The Covid Impact to Public Healthcare Utilization Among Urban Low-Income Subsidized Community in Klang Valley Malaysia. Retrieved from: https://journals.sagepub.com/doi/full/10.1177/23333928211002407
2United Nations (2015). Transforming our World: the 2030 Agenda for Sustainable Development. Retrieved from: https://sdgs.un.org/2030agenda
3United Nations (2019). Accelerating Towards a Fairer Future. Retrieved from: https://news.un.org/en/story/2019/12/1054411
4Falcon, D. (2019) The Health Care Gap in Rural Malaysia. Retrieved from: https://preserve.lib.lehigh.edu/islandora/object/preserve%3Abp-15927768
5Ibid.
6Ministry of Health Malaysia (2020). Strategic Framework of the Medical Programme. Retrieved from: https://www.moh.gov.my/moh/resources/Pelan_Strategik_KKM.pdf
7International Trade Administration (2020). Malaysia Healthcare. Retrieved from: https://www.trade.gov/market-intelligence/malaysia-healthcare
8Ministry of Finance Malaysia (2020). Bernama – Budget 2021: RM31.9 Bln Allocated To Health Ministry More Than Last Year – Zafrul. Retrieved from: https://www.mof.gov.my/en/news/press-citations/bernama-budget-2021-rm31-9-bln-allocated-to-health-ministry-more-than-last-year-zafrul
9United Nations Economic and Social Commission for Asia and the Pacific. Spatial Analysis: Ageing Population of Multi-ethnic in Rural Area, Malaysia. Retrieved from: https://www.unescap.org/sites/default/files/70_Spatial_Analysis_Ageing_Population_of_Multi-ethnic_in_Rural_Area_Malaysia.pdf
10The BMJ (2001). Point of Care Testing. Retrieved from: https://www.bmj.com/content/322/7297/1285














