5 Key Lessons the World Must Learn to Combat Infectious Diseases
1. Out of Sight Should Not Be Out of Mind
Infectious diseases have been cast as a terrifying new threat. This is despite the fact that humankind has lived surrounded by viruses for thousands of years. When pandemics fade, so do our memories.
This ‘out of sight, out of mind’ mindset has to change. Preparation in the aftermath of disease outbreaks is what will shield us in the next one.
Policymakers now realise the danger posed by infectious agents — not just viruses, but also the multi-drug resistant bacteria. This sustained awareness and interest in the management of infectious diseases, heightened because of COVID-19, must continue.
While there is no doubt that the impact of COVID-19 has been much more virulent in comparison to SARS, we should be prepared for what could be an even more devastating outbreak in the next decade — potentially more contagious and with a higher mortality rate. It could be an existing disease such as swine flu, polio, zika, or a totally unknown pathogen.
Such a threat is already lurking in our own backyard — whether it is the Pulau virus, Tioman virus or Melaka virus. These bat viruses can cause infections in humans. The only thing that is stopping a new infection is the inability of these viruses to spread quickly and easily, as they have not adapted to humans — yet.

2. A Problem of This Magnitude Requires Funding to Match
Despite greater awareness, there is a dearth of money to support prevention and control endeavours. Investments are needed to develop technologies that can identify these viruses including the adoption of artificial intelligence tools, for isolation facilities to house infected individuals, and for preventive measures is key to creating an integrated epidemic prevention system.
It’s also important not to look at these investments in a vacuum, as they can be invaluable for a multitude of scenarios. Purpose-built hospitals can be used to treat cases of antibiotic resistant bacteria during peace time, and repurposed when outbreaks occur.
Similarly, countries should not ignore the importance of preemptive efforts. We have witnessed the chaos that descended on health systems worldwide because of the inadequate stockpile of protective gear for healthcare workers, and the protectionist stance adopted by several countries.
We need to remember that any one country remaining vulnerable to COVID-19 or other disease outbreaks puts the whole world in peril.
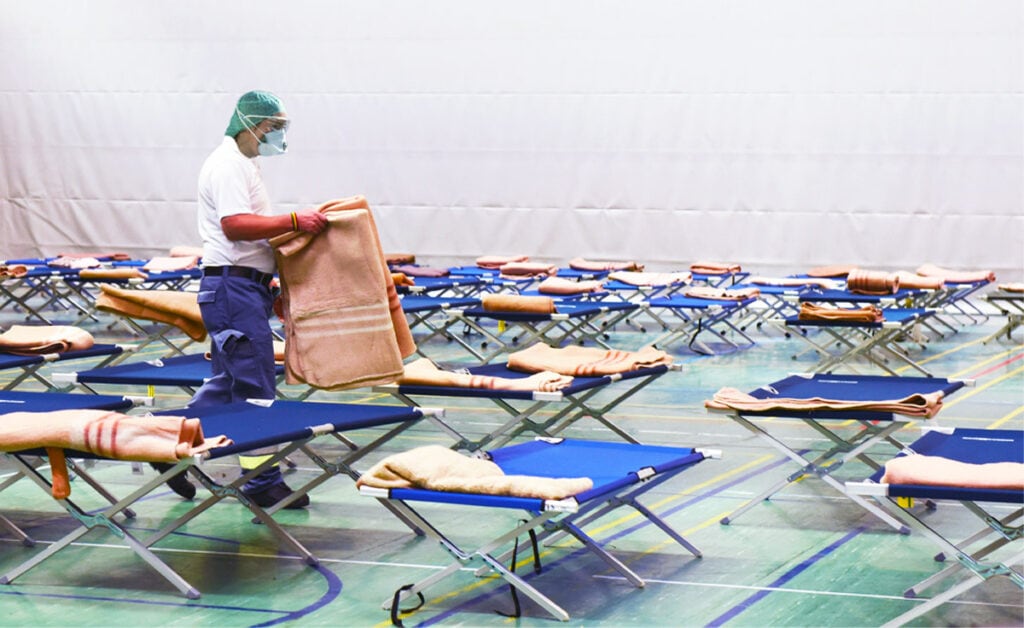
3. We Must Rely on the Proven Success of Science-led Decisions
Countries that have done relatively well in limiting community transmission and safeguarding the health of citizens were those that were better prepared. These health systems of countries such as Singapore, China, Hong Kong, Taiwan and South Korea, to name a few, are often the ones that have had prior experience with SARS or MERS.
But prior experience needs to be supported with a robust learning model. Implementing measures based on clinical evidence and rooted in science, rather than hearsay, can make a tremendous difference. The never-ending cycle of outbreaks-surveillance-containment is a resource-intensive exercise that no country can sustain in the long-term. This is where information sharing and use cases can help empower countries to learn from one another.
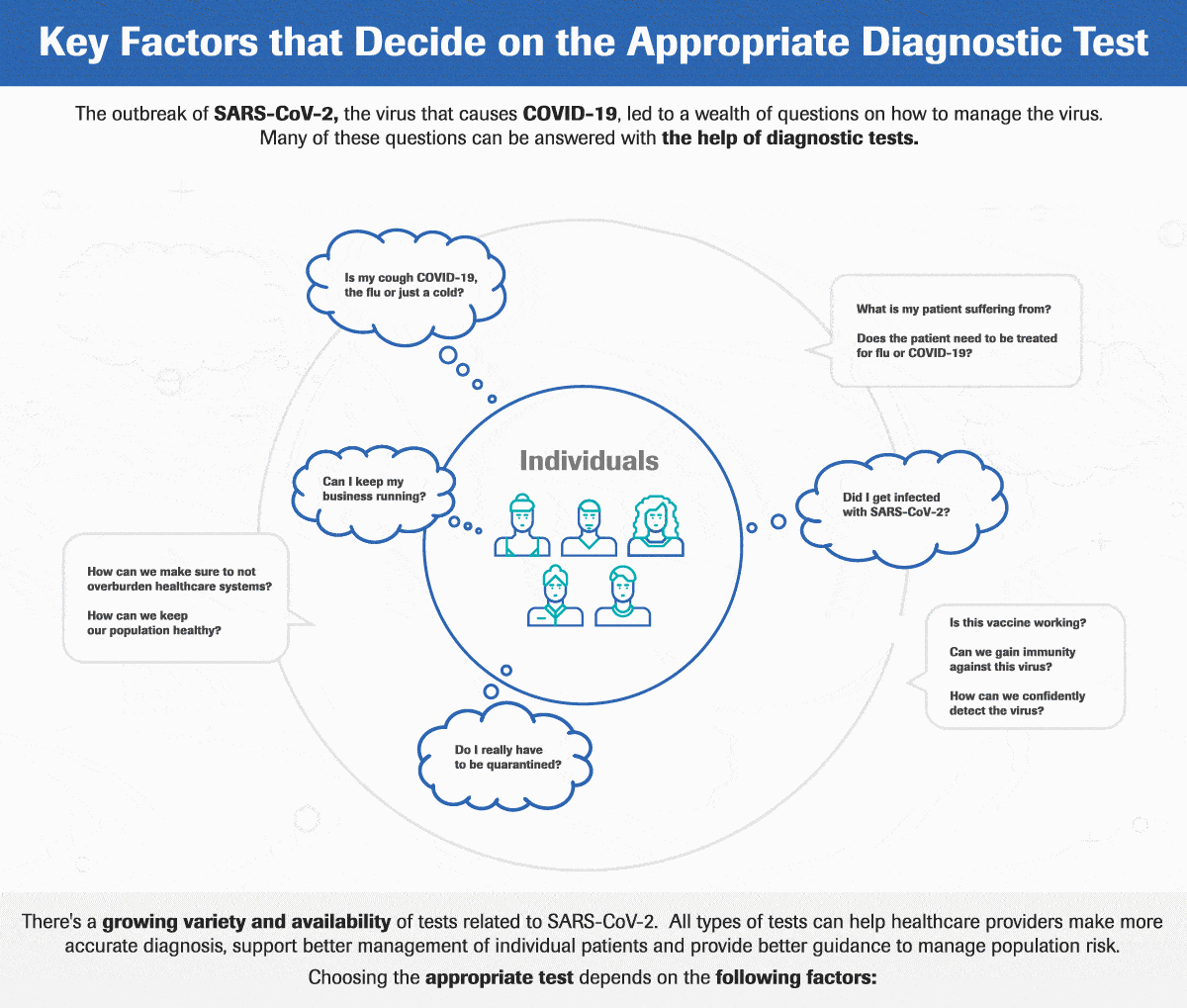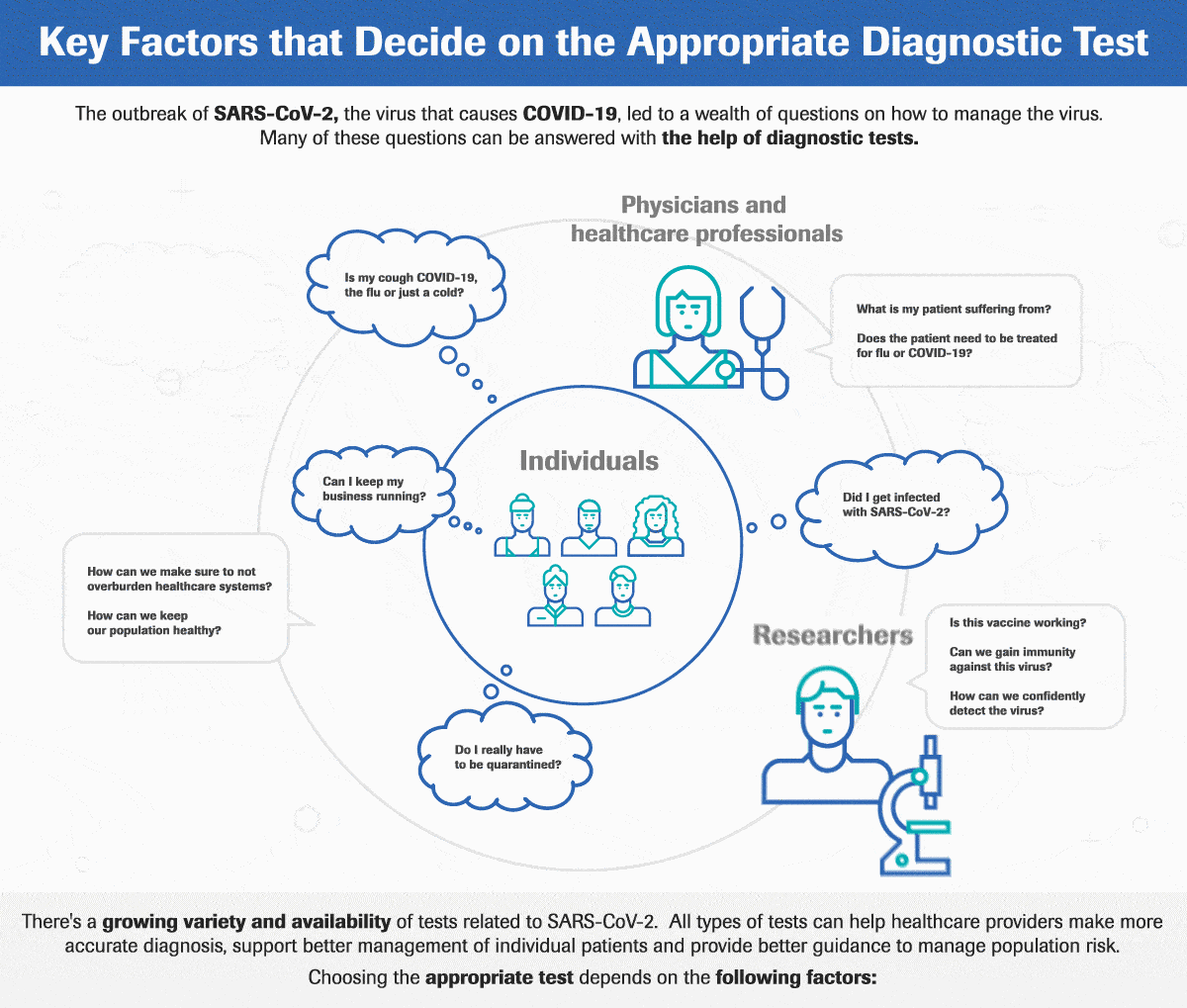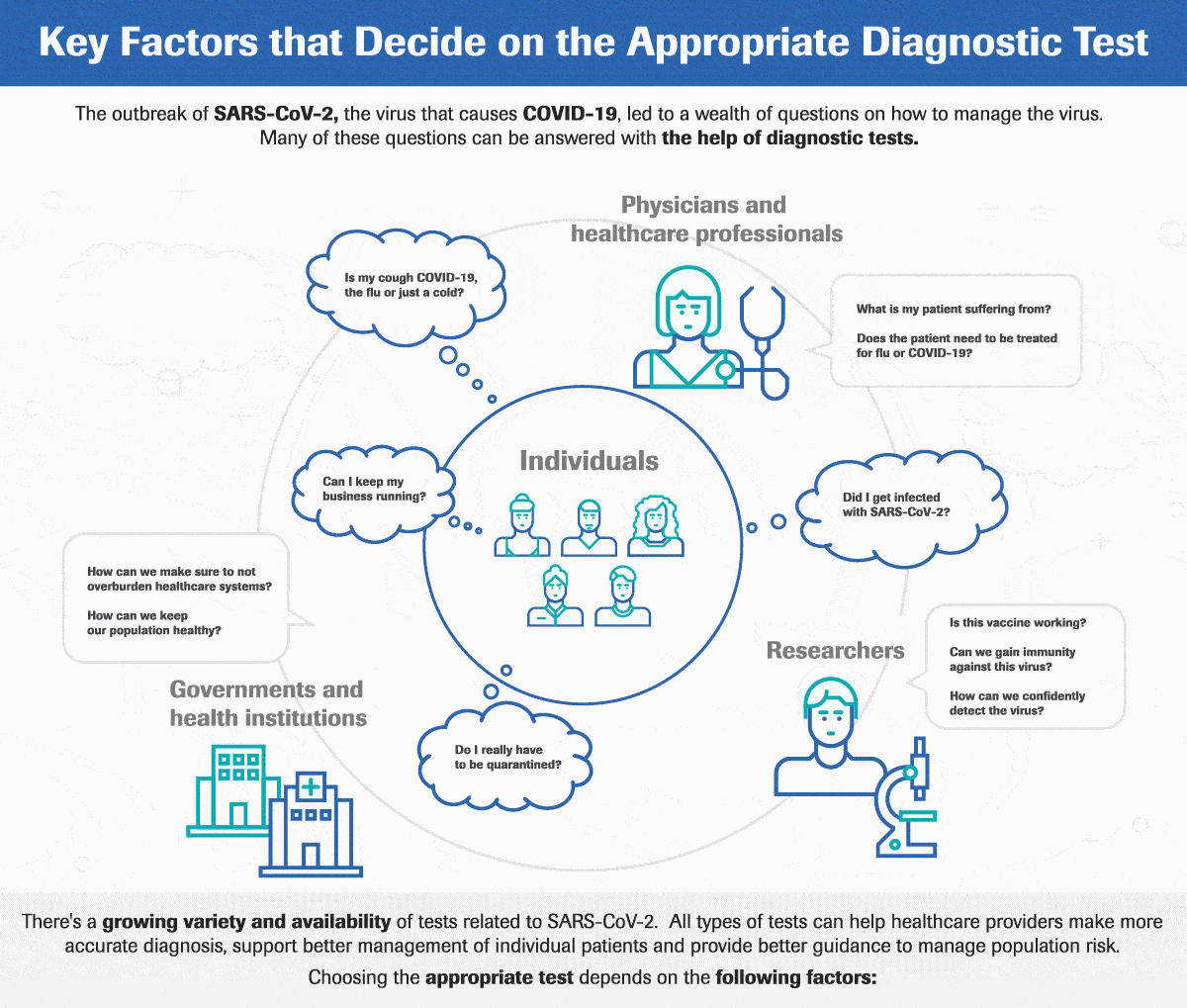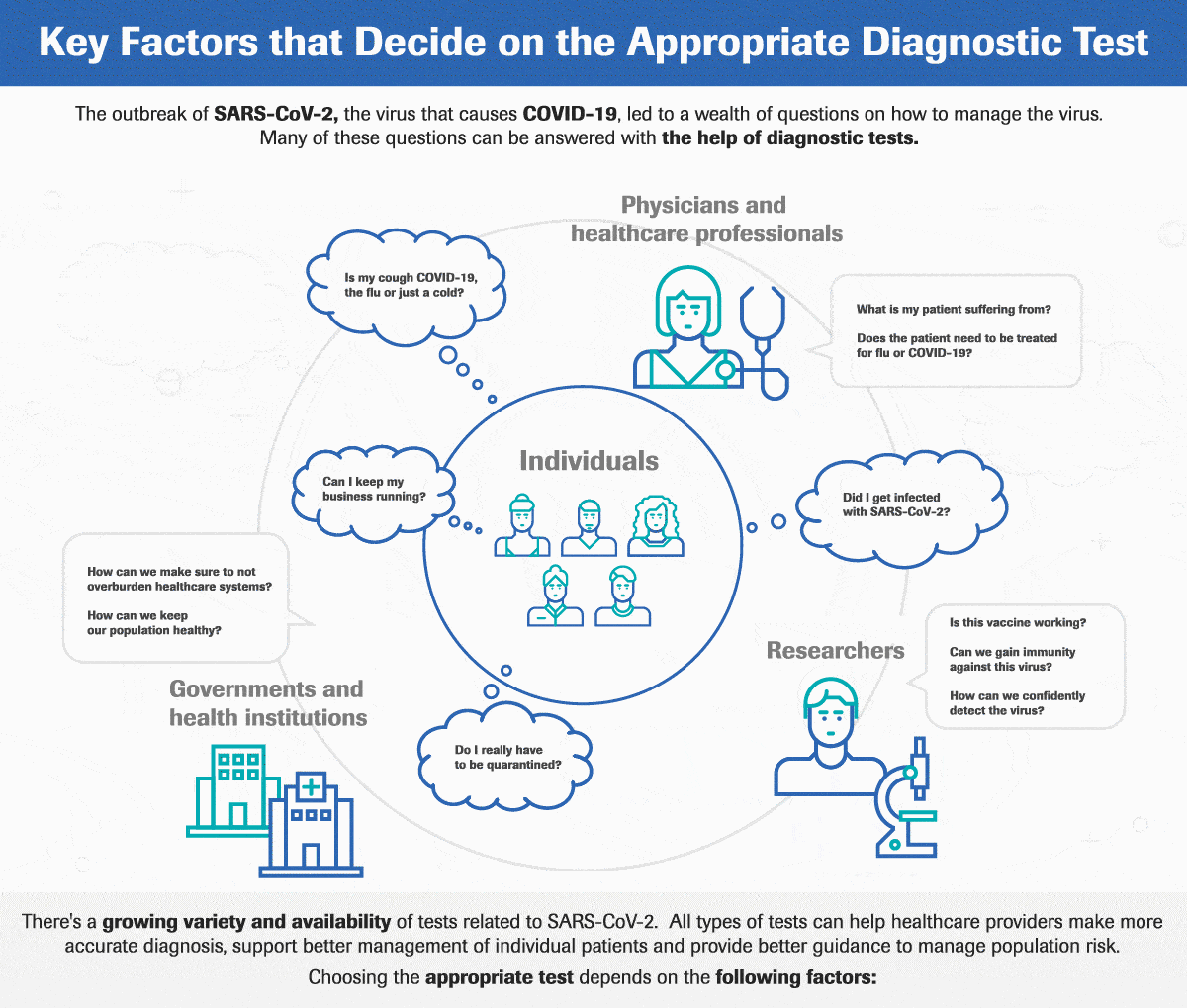
4. We Cannot Overcome Healthcare Manpower Challenges Without Digital Technology
An integrated epidemic prevention and control can protect lives and livelihoods, thereby lessening the fallout from an economic downturn. But this is a costly and labour-intensive proposition. Increasing the number of healthcare workers alone is not a sustainable solution. The burden of diseases and patient population is growing too rapidly for us to catch up. Digital tools like artificial intelligence can help.
However, we must have legislation in place that enables the adoption of such tools, much before the next outbreak. There are justifiably concerns around privacy and individual rights that need be debated within the context of the good of individuals versus national interest.

5. Rebuild Healthcare with a Solid Foundation
Diagnostics plays a very important part in national health strategies. We saw many countries initially struggling without diagnostic tests that could accurately confirm COVID-19 infections. Every single day of delay leads to more transmission. Every day you cannot identify your enemy with the test is another day you can’t aim your ammunition at it.
Once effective diagnostic tests became available, the second hurdle was to ramp testing up quickly — procuring test kits in the middle of a global public health crisis, with travel routes closed, was extremely difficult.
Outbreak preparedness requires foresight and planning to avert worst-case scenarios. Building the necessary infrastructure, evolving testing strategies (such as exploring when a centralised versus decentralised testing approach works best) and determining emergency approval protocols to reduce bureaucratic hurdles in advance can strengthen our response.















