Hans, as an industry expert and healthcare policy advisor, what do you feel is the real value of diagnostics for the healthcare ecosystem?
Whether it’s infectious diseases or chronic health conditions, a large part of the value of diagnostics information lies in prevention, early detection and management. In Europe, in vitro diagnostic (IVD) testing provides critical information from prognosis and screening to disease progression and treatment pathways, enabling healthcare providers to make the best decisions on expected courses of action — with minimised uncertainty.
For example, early and accurate diagnosis can help identify changes in the body even before the disease occurs,1 buying clinicians time to make optimal treatment choices for patients. Ongoing patient monitoring helps physicians measure treatment effectiveness, potentially preventing or slowing disease progression.
But for healthcare delivery to realise its full potential, diagnostic information needs to be captured, assessed and gleaned for insights that can inform patient care decisions. This improves diagnoses, aids in disease prevention and enables large-scale monitoring of symptoms. Most importantly, the data can be used to improve health management in our societies by influencing policy decisions made at the national, or even regional, level.

Do you feel the value of diagnostics in healthcare is sufficiently appreciated?
Currently, there is not enough consideration of the value that diagnostics bring to the table. In Europe for example, we spend an average of only 2.8 percent2 of the healthcare budget on early detection and prevention; most European Union (EU) member states spent an average of more than 50 percent3 of their healthcare budgets on curative and rehabilitative care services.
I would say that the same thing is happening in Asia-Pacific (APAC) right now. Governments tend to view diagnostics as a cost, which is why healthcare policies tend to gravitate towards cost containment and protectionist measures rather than leaning on value or evidence-based assessments that can more accurately demonstrate the true value of diagnostics — for the individual and for society.
To give a personal anecdote, early diagnosis is one of the reasons why my wife is alive today, because her cancer was detected right from the very beginning, which expanded the range of treatment possibilities available to her. Only with frequent and early testing can we can begin to extract the full value of diagnostics.
How can diagnostic information help make health systems more resilient, in the era of COVID-19?
The pandemic has shown that not only is diagnostic data undervalued, it is underutilised. We still understand very little about the coronavirus, and it is a shame that we’re not leveraging the copious amounts of tests being done on a daily basis to better formulate our clinical responses to COVID-19. For instance, is there a way for us to integrate patient data with existing biomarkers to explain the difference in symptom severity?
Having said that, I believe that COVID-19 has made the case for value-based healthcare (VBHC) stronger than ever. The additional resource pressures under which our health systems continue to operate at present is a compelling catalyst for us to begin transitioning to such a model. Even before the pandemic, the World Health Organization (WHO) estimated that between 20 and 40 percent of all global health spending is currently wasted through inefficiency.4
Widespread adoption of value-based care can reduce that number. By employing incentives that reward healthcare providers for improving patient health, we can benefit from the societal gains of early detection and prevention of disease progression, such as the more efficient use of scarce resources and cost savings.
When health systems consider the entire patient journey holistically, they utilise diagnostic information gathered at various touch points to inform and improve patient experience.

What needs to be in place for value-based care to become a reality, and drive the healthcare of the future?
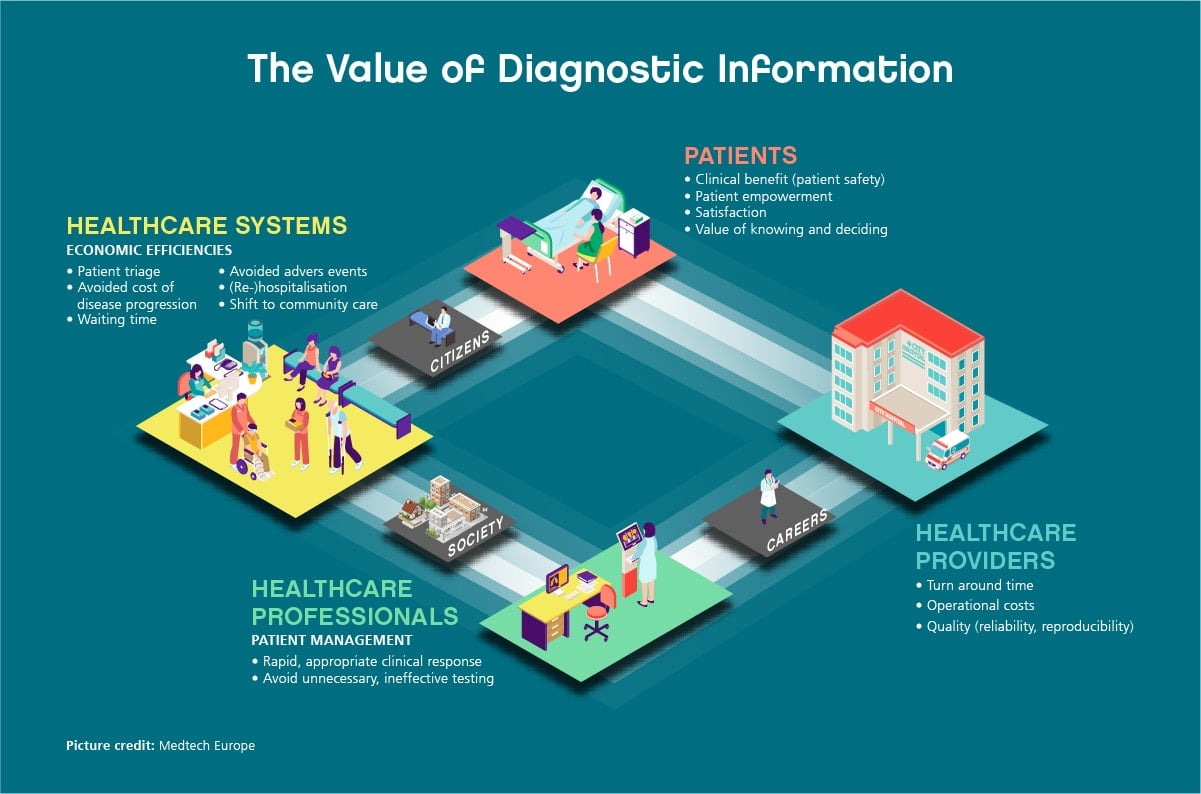
There is a need for a new evaluation framework, one that goes beyond conventional cost containment approaches to focus on the full breadth of value that diagnostic information can provide. MedTech Europe has captured this in its Value of Diagnostic Information (VODI) framework to help policymakers, healthcare providers, payers and procurers recognise how the value of this diagnostic information should be assessed and reimbursed.
To achieve VODI, we will need to begin by introducing relevant and pragmatic assessment methodologies that go beyond mere technological criteria. Start by engaging with value-based systems and reviewing current financing models to favour longer-term investment cycles and true societal value. Policymakers should consider fostering cross-boundary data sharing for regional, value-driven healthcare models, while industry and providers should collaborate on win-win partnerships to bring products to market quicker.
Ultimately, we must forget our old-fashioned concept of cost in healthcare and begin to examine the value of diagnostics by looking at its returns. Not just monetarily, but in terms of its full impact on health systems and societies.
When we do this, we redefine healthcare in a way that transcends simply treating the sick.
Diagram Dialogues
Subscribe to our podcast to hear expert insights from the world of diagnostics
References:
1American Cancer Society. Cervical Cancer Early Detection, Diagnosis, and Staging. Retrieved from https://www.cancer.org/content/dam/CRC/PDF/Public/8601.00.pdf
2Eurostat (2021). Healthcare expenditure statistics. Retrieved from: https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Healthcare_expenditure_statistics#Healthcare_expenditure_by_function
3Ibid.
4World Health Organization. More health for the money. Retrieved from: https://www.who.int/whr/2010/10_chap04_en.pdf














